Menopause: Practical Help for Symptoms, Sleep, Mood, and Health
Menopause brings big changes fast and slowly. Hot flashes, night sweats, irregular periods, mood swings, and vaginal dryness are common. You might also notice weight shifts, sleep problems, or changes in blood sugar if you have diabetes. This page gives clear, practical steps to feel better and know when to see a clinician.
Treatment options
Hormone replacement therapy (HRT) often reduces hot flashes and protects bones. HRT can be pills, patches, gels, or rings. It works best when tailored to your age, health, and family history. If HRT isn’t right, non-hormonal drugs can help: low-dose antidepressants, gabapentin, or a blood pressure medicine called clonidine. Vaginal dryness responds well to local estrogen creams, rings, or non-hormonal moisturizers and lubricants.
Daily habits that help
Small daily choices cut symptoms a lot. Dress in layers and pick breathable fabrics for hot flashes. Keep a cool bedroom, use a fan, and avoid heavy blankets at night. Limit spicy food, caffeine, and alcohol before bed. Try paced breathing or brief relaxation exercises when a hot flash starts. For sleep, set a consistent bedtime, reduce screens an hour before sleep, and avoid large meals late at night.
Talk to your doctor about bone health. Menopause speeds bone loss. Get a bone density test if recommended. Aim for regular weight-bearing exercise like walking or light strength training three times a week. Make sure you get enough calcium and vitamin D from food or supplements. Also check blood pressure and cholesterol—menopause can affect heart risk.
Mood swings and brain fog are common. Keep a simple routine, sleep well, and stay active. Talk therapy helps; so do support groups or online forums. If mood or anxiety is severe, medications and counseling work well. If you’re on diabetes meds, watch for changes in blood sugar with mood swings or sleep loss.
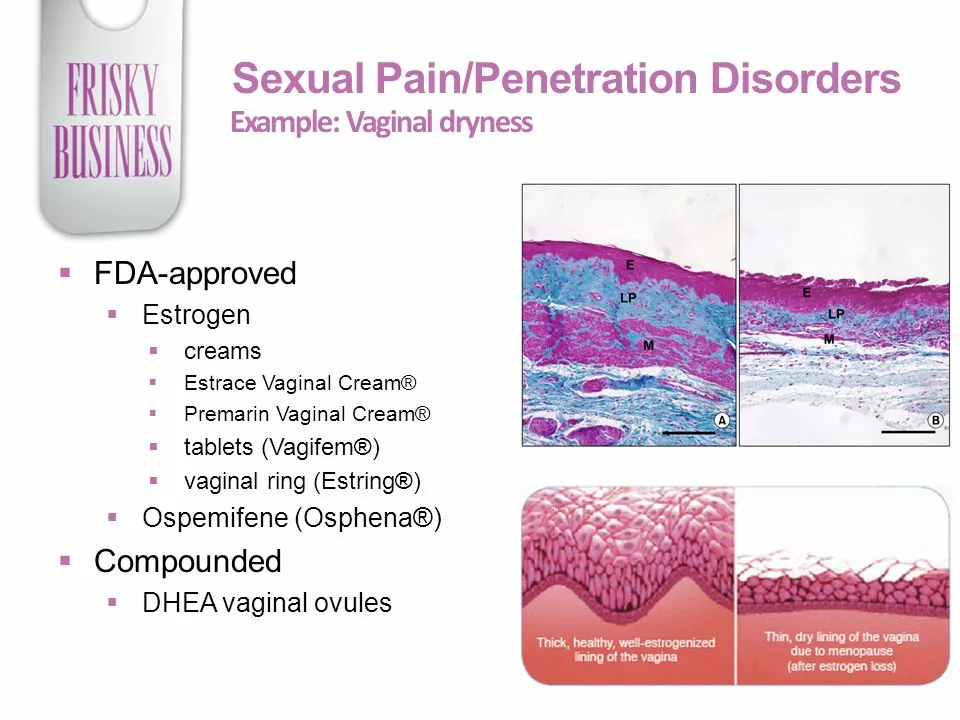
Vaginal dryness and pain during sex are fixable. Over-the-counter lubricants help right away. Regular sexual activity or pelvic floor exercises can improve comfort and blood flow. For persistent pain, a pelvic exam and tailored treatment help. Talk openly with your partner and your clinician about changes you notice.
See a clinician if bleeding returns after 12 months without periods, if bleeding is heavy or irregular, or if hot flashes disrupt daily life. Also see a doctor for sudden weight gain, severe mood changes, or symptoms that worry you. If you have diabetes, ask for help adjusting medication as hormone levels change. Bring a list of symptoms, medications, and any questions to your visit.
Keep routine screening up to date: mammograms, cervical screening where recommended, and bone density tests if your doctor suggests them. Check blood sugar, A1C, lipids, and blood pressure more often if symptoms change. Write down changes to share at appointments so nothing gets missed.
Start small: track hot flashes and sleep for two weeks, note what triggers them, and try one change at a time. If you smoke, quitting helps symptoms and heart health. Use this site to find articles, but always check treatments with your own clinician before starting anything new.
Menopause and Vaginal Dryness: Solutions for Comfort
Haig Sandavol Apr 29 14Menopause and vaginal dryness can be a challenging issue for many women, but luckily there are solutions for comfort. In my latest blog post, I discuss the various options available, such as using water-based lubricants, vaginal moisturizers, and hormone therapy. I also explore natural remedies and lifestyle changes that can help combat dryness and improve overall vaginal health. Join me in learning about these effective measures to maintain comfort and confidence during this significant transition in a woman's life.
More Detail