Vaginal Dryness: What’s Causing It and What You Can Do
Vaginal dryness is common and annoying. It can make sex painful, cause itching or burning, and increase infections. The good news: most causes are treatable, and simple changes often bring fast relief.
So why does it happen? Low estrogen is the top reason — think menopause, breastfeeding, or surgical removal of ovaries. But other causes include certain medicines (antidepressants, antihistamines), smoking, stress, and chronic conditions like diabetes. High blood sugar can change vaginal mucus and raise the risk of yeast and bacterial infections, which can feel dry or irritated.
Quick fixes you can try today
Start with nonprescription options. Water-based lubricants are great for sex; they reduce pain and wash out easily. For daily comfort, try a vaginal moisturizer — these hydrate tissue and last longer than lubricants. Look for products with hyaluronic acid or glycerin if you tolerate them well. Avoid scented products, douches, and harsh soaps; they irritate delicate tissue.
If you use condoms, avoid oil-based lubricants (they can weaken latex). Try a silicone-based lubricant for longer-lasting slipperiness during sex, but test it on your skin first if you have sensitivities.
When to consider medical treatments
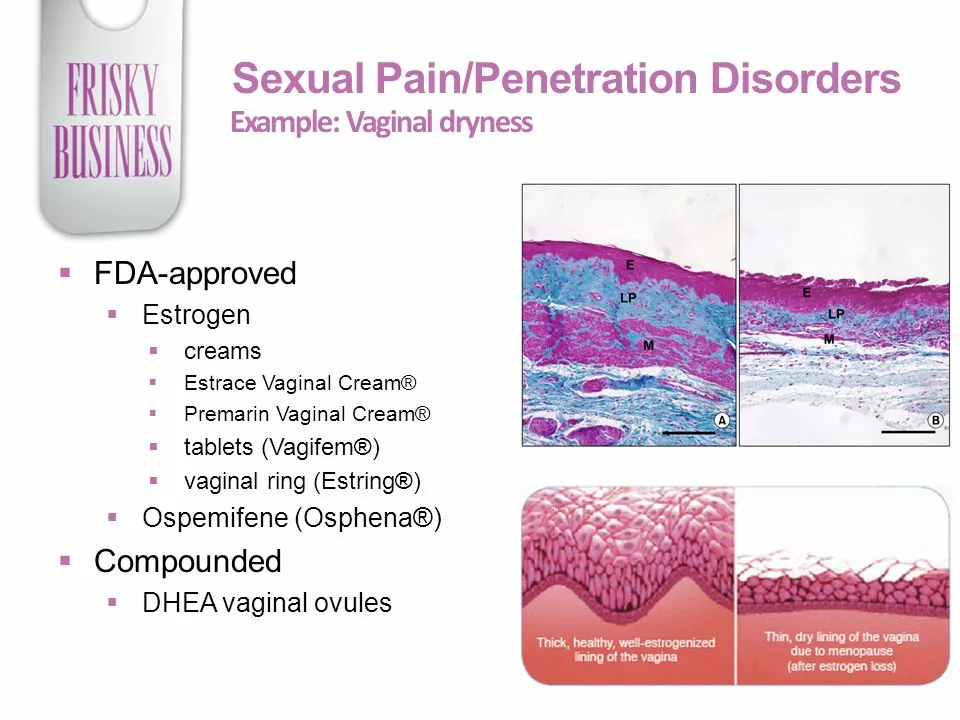
If OTC measures don't help, talk to your clinician about prescription options. Low-dose vaginal estrogen (cream, tablet, or ring) restores moisture and tissue health with minimal systemic exposure for many women. There are also non-hormonal prescription choices, like ospemifene or vaginal DHEA, which some women find helpful. Your provider can weigh risks based on your health history.
For women with diabetes, managing blood sugar often eases symptoms and lowers infection risk. If yeast or bacterial infections keep coming back, get tested and treated — repeated infections can worsen discomfort and dryness.
Pelvic floor physical therapy helps if tight muscles make sex painful. Counseling or couples therapy can help when dryness affects intimacy or causes anxiety.
Know the red flags: heavy bleeding, severe pain, a new lump, or symptoms that don't improve after treatment need prompt evaluation. Also see a doctor if dryness started after cancer treatment; some cancer therapies require special care and different treatment choices.
Questions to ask your provider: Could my medicines cause this? Is vaginal estrogen safe for me? What product do you recommend for daily use? When should I return if this doesn't improve?
Small changes add up: stop smoking, choose breathable cotton underwear, avoid tight pants, stay hydrated, and keep blood sugar under control if you have diabetes. With the right mix of lifestyle swaps and medical help, most women regain comfort and confidence quickly.
Menopause and Vaginal Dryness: Solutions for Comfort
Haig Sandavol Apr 29 14Menopause and vaginal dryness can be a challenging issue for many women, but luckily there are solutions for comfort. In my latest blog post, I discuss the various options available, such as using water-based lubricants, vaginal moisturizers, and hormone therapy. I also explore natural remedies and lifestyle changes that can help combat dryness and improve overall vaginal health. Join me in learning about these effective measures to maintain comfort and confidence during this significant transition in a woman's life.
More Detail