Stem cell transplants: what they are and what to expect
Thinking about a stem cell transplant? You’re not alone—these procedures can change outcomes for blood cancers, bone marrow failure, and some autoimmune conditions. This page gives plain, practical info so you can talk to your doctor with confidence.
What a stem cell transplant actually is
Put simply, a stem cell transplant replaces damaged or missing blood-forming cells. Doctors first give treatments like chemo or radiation to wipe out the disease. Then they infuse healthy stem cells that restore the bone marrow. Those new cells grow into red blood cells, white blood cells, and platelets.
There are two main types: autologous (your own cells) and allogeneic (someone else’s cells). Autologous transplants use your cells to reduce immediate rejection risk. Allogeneic transplants use a donor and can offer a stronger anti-disease effect, but they bring extra risks like graft-versus-host disease (GVHD).
What to expect before, during, and after
Before: You’ll have tests—blood work, heart and lung checks, infection screens, and HLA typing if a donor is needed. Ask about fertility preservation, vaccines, and dental checks. Pack for a long hospital stay and arrange a support person for home recovery.
During: Conditioning (chemo +/- radiation) lasts days to a week. The transplant itself is usually an infusion through a central line—quick and similar to a blood transfusion. The worst days are often the first few weeks when your immune system is very low.
After: Engraftment (when new cells start working) can take 2–4 weeks. Expect frequent blood tests, infection precautions, and possibly transfusions. If you had an allogeneic transplant, you may need immunosuppressants to prevent GVHD. Recovery can take months; full immune recovery sometimes takes a year or more.
Risks to watch for: infections, bleeding, organ stress from conditioning, GVHD after donor transplants, and disease relapse. Your team should explain the specific risks for your diagnosis and health profile.
How donors are matched: For allogeneic transplants, doctors match human leukocyte antigens (HLA). Sibling matches are best, but unrelated donors or cord blood can work. Matching reduces GVHD risk and improves success chances.
Questions to ask your team: What are my success and relapse rates? Why this transplant type for me? What side effects are most likely? How long will I stay in hospital? What follow-up care and vaccines will I need? Should I consider clinical trials?
Who is a candidate: Age, overall health, other medical problems, and disease stage matter. Some older adults and people with comorbidities may still be candidates with adjusted plans—ask your specialist directly.
Want to learn more? Look for patient guides from transplant centers and clinical trial listings. If you have diabetes or other chronic conditions, tell your transplant team so they can tailor care. A stem cell transplant is a big step, but clear info and a good support plan make it manageable.
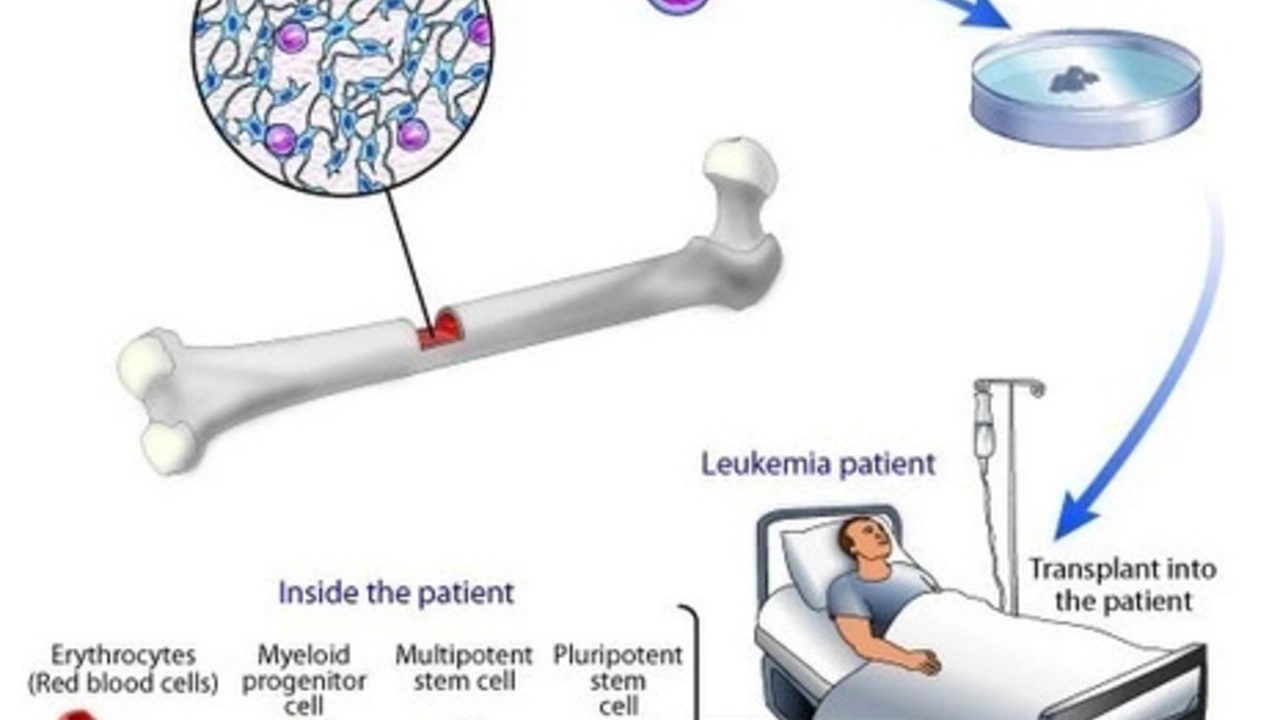
The Role of Stem Cell Transplants in Cancer Treatment
Haig Sandavol Jul 1 13Stem cell transplants have emerged as a promising tool in cancer treatment. These transplants help replace bone marrow that's been damaged or destroyed by cancer. They can either come from the patient's own body or from a donor, aiming to give the body a new, healthy start. This procedure can be a game-changer, especially for patients with blood-related cancers like leukemia. It's not without risks though, so it's important to thoroughly discuss these options with your healthcare provider.
More Detail