Epigastric pain: what it is and what to do now
Feeling a sharp, dull, or burning ache just below your ribs in the middle of your upper belly? That's epigastric pain. It can come on after a heavy meal, at night, or suddenly and severely. Most of the time it’s caused by benign issues like acid reflux or gas, but some causes need medical care. This guide helps you decide when to try simple fixes and when to get help.
Common causes you should know
Here are the things doctors see most often:
- Acid reflux or heartburn: a burning feeling that often gets worse when you lie down or bend over.
- Gastritis or peptic ulcer: pain that can be constant or come in waves, sometimes linked to eating or certain medicines like NSAIDs.
- Gallbladder problems: pain may start in the epigastric area then move to the right side and can follow fatty meals.
- Pancreatitis: a severe, steady pain that often radiates to the back and may come with nausea and vomiting.
- Functional dyspepsia or gas: bloating and fullness with mild to moderate pain.
- In people with diabetes: delayed stomach emptying (gastroparesis) can cause fullness and upper abdominal pain after meals.
When to get urgent care
Head to the ER or call your doctor right away if you have any of these:
- Very severe, sudden pain;
- Pain with fever, persistent vomiting, or unable to keep liquids down;
- Shortness of breath, sweating, or pain spreading to the jaw or left arm (possible heart attack);
- Blood in vomit or black/tarry stools;
- Jaundice (yellowing of skin or eyes) or fainting.
For milder, new pain, book a same-week appointment so a clinician can check you over and order tests if needed.
Simple things to try at home: avoid alcohol and spicy or fatty foods, eat smaller meals, stop NSAIDs if you can, try an over-the-counter antacid for short-term relief, and avoid lying flat right after eating. If you have diabetes, keeping blood sugar steady often helps reduce stomach symptoms.
Typical tests your doctor may order include blood work (to check for infection, liver or pancreatic problems), abdominal ultrasound (good for gallbladder issues), and endoscopy (to look at the stomach lining and check for ulcers or H. pylori infection). Treatment depends on the cause: antacids or proton pump inhibitors for reflux, antibiotics plus acid therapy for H. pylori, IV fluids and monitoring for pancreatitis, or surgery for problematic gallstones.
If pain is recurring or affecting daily life, don’t ignore it. Keep a short diary: what you ate, when pain started, other symptoms, and any medicines you’re taking. That makes clinic visits faster and more useful. Epigastric pain is common, but with the right steps you can often find relief fast and avoid complications.
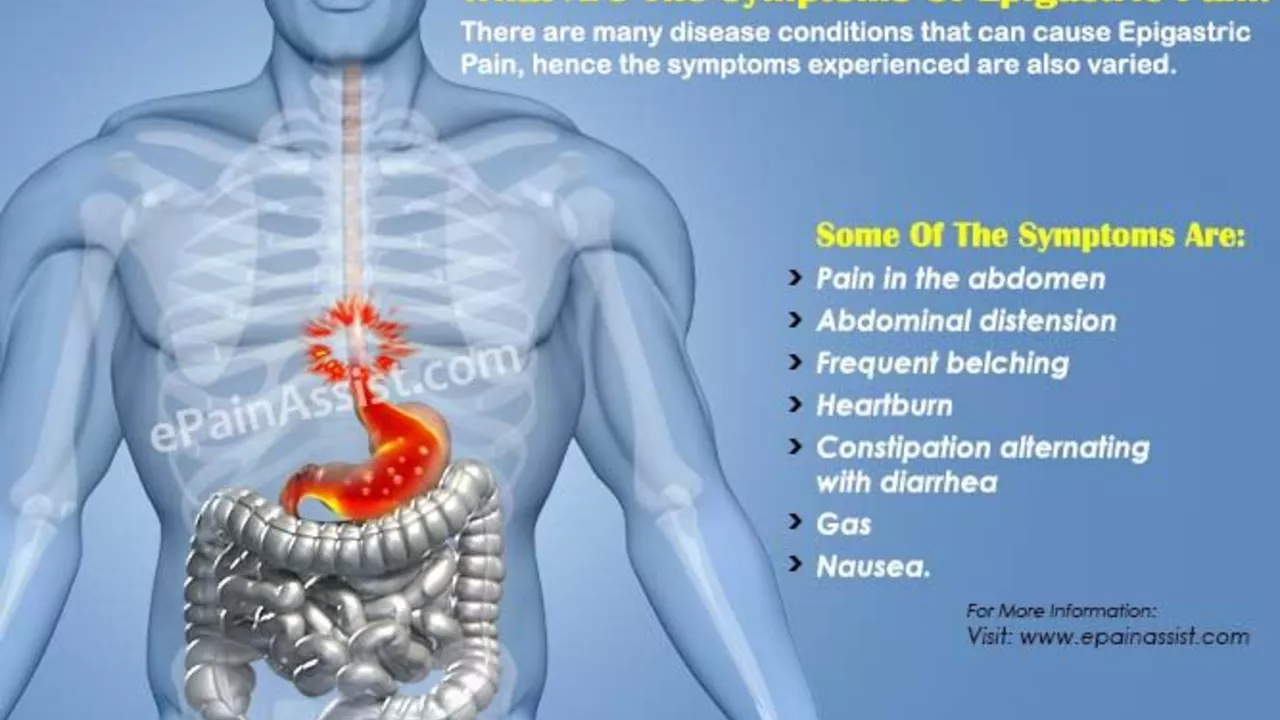
Epigastric Pain and Acid Reflux: Tips for Managing Symptoms
Haig Sandavol Aug 1 14Belly battles are no fun, mate! Epigastric pain and acid reflux, the dynamic duo of discomfort, often go hand in hand. But don't panic, I've got some handy tips to help you fight back. From dietary changes to lifestyle modifications, there are several tactics you can employ to keep these pesky problems in check. So, sit tight, as we dive into the world of managing these fiery foes, promising a smoother journey down your food pipe!
More Detail