Digestive disorders — what to watch for and what actually helps
Gut problems can show up as a dull ache, sudden pain, bloating, nausea, or weird bowel changes. Some things are minor and clear up fast. Others need a doctor or different medicines. This page helps you tell the difference, explains common treatments, and gives quick, practical tips for safer medicine use.
Common causes and clear warning signs
Most digestive complaints come from three things: diet and lifestyle, infections, or medication side effects. Overeating, fatty food, or too much alcohol can cause reflux, bloating, and indigestion. Bacterial or parasitic infections often bring sharp pain, fever, and diarrhea. Some medicines — like metoclopramide — help digestion but can cause mood or movement side effects in some people.
Know when to see a doctor: severe belly pain, persistent vomiting, blood in stool or vomit, high fever, sudden weight loss, or dehydration. If symptoms are mild but last more than a week, get a checkup. Quick action prevents small problems from becoming big ones.
Treatment basics, medicines, and shopping smart
First-line fixes are simple: hydrate, rest, cut spicy and fatty foods, and try a bland diet for a few days. Over-the-counter antacids or acid reducers can ease heartburn. For infections, antibiotics may be needed — for example, metronidazole (Flagyl) is common for some gut infections, but there are valid alternatives depending on the bug and allergies.
Prescription drugs like metoclopramide can speed stomach emptying but watch for side effects. Recent coverage on our site explains how metoclopramide can affect mood and what to tell your doctor if you notice changes. If you’re prescribed a long-term blood pressure or other medicine, ask how it might affect digestion — some drugs change bowel habits or appetite over time.
Shopping for meds online? Be cautious. Use licensed pharmacies, check reviews, and confirm you need a prescription for prescription-only drugs. We have guides on safe online buying and comparisons of antibiotic alternatives that can help you make informed choices.
Practical everyday steps: keep a food diary to spot triggers, try smaller meals, reduce caffeine and alcohol, and consider a short course of probiotics if you have antibiotic-related diarrhea. If you use antibiotics, follow the full course and talk to your provider about resistance risks and alternatives when needed.
Want more detail? Read our posts on metoclopramide’s mental health effects, Flagyl alternatives, and the recent rise in gut infections after heatwave and seasonal changes. Those articles dive into risks, alternatives, and safe use so you can manage symptoms without guesswork.
Got specific symptoms or a medicines list? Bring them to your next appointment — a focused checklist helps your doctor pick the safest, simplest fix fast.
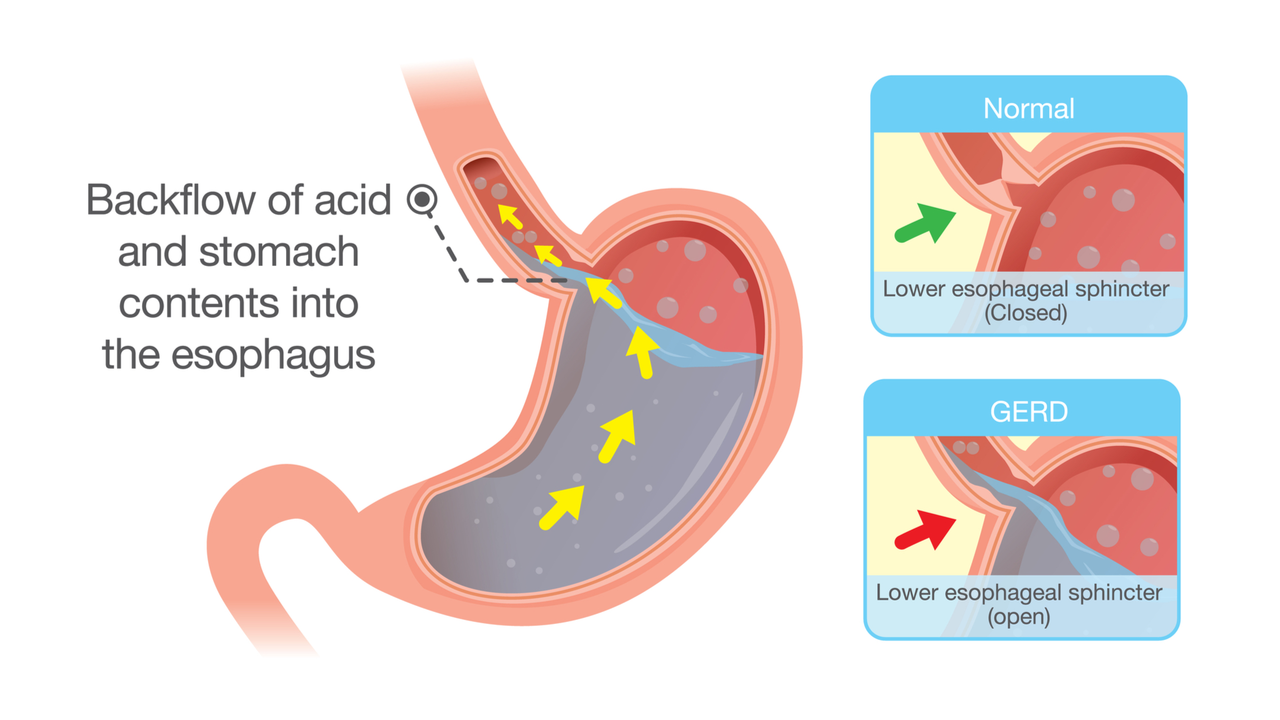
GERD and Acid Reflux: Understanding the Differences Between These Digestive Disorders
Haig Sandavol Jun 12 6As a blogger, I've come to realize the importance of understanding the differences between GERD and acid reflux, two common digestive disorders. While both involve stomach acid flowing back into the esophagus, GERD is a chronic condition characterized by frequent acid reflux episodes. Acid reflux, on the other hand, is an occasional occurrence that can be triggered by certain foods or lifestyle factors. By being aware of these distinctions, we can better manage our digestive health and seek appropriate treatment when necessary. Stay tuned for more insights on these conditions and how to keep them in check!
More Detail