Central (Cranial) Diabetes Insipidus — What You Should Know
Central (cranial) diabetes insipidus is a condition where your body can't hold onto water because it lacks enough antidiuretic hormone (ADH). That hormone comes from the pituitary. Without it, your kidneys pour out very dilute urine and you feel extremely thirsty. This sounds simple, but the daily impact can be big — waking up many times at night, needing water constantly, or getting dehydrated quickly during illness.
Symptoms and causes
The most common signs are passing large volumes of clear urine and being very thirsty. You might wake several times overnight to drink. Babies and older adults can show dehydration, low weight gain, or confusion. Causes range from head injuries, pituitary surgery, and tumors to autoimmune problems and infections. Sometimes no clear cause shows and doctors call it idiopathic. If you had recent brain surgery, trauma, or radiation near the pituitary, ask your team about this risk.
Diagnosis and treatment
Doctors start with simple tests: check how much urine you make, measure your urine and blood concentration (osmolality), and test sodium levels. A water deprivation test is sometimes done to see if urine concentrates when you don’t drink. An MRI of the brain looks for pituitary damage or tumors. Treatment aims to replace the missing hormone and protect your body from losing too much water. The main medicine is desmopressin (DDAVP). It comes as a nasal spray, tablet, or injection. Your doctor will pick the dose and form that fits your life. Watch for overcorrection — taking too much desmopressin can cause low sodium and swelling. That’s why periodic blood tests matter, especially after starting or changing dose.
Practical tips that help day to day: carry a water bottle and sip regularly, track how much you drink and pee if you’re starting treatment, and wear a medical ID if you have severe disease. If you travel, pack extra medication and copies of prescriptions. During fever or vomiting, your fluid needs change — call your doctor early.
If you or a family member has sudden, extreme thirst or very wet diapers in a baby, seek medical attention. Also get help if you feel dizzy, faint, or unusually weak — those are signs of dehydration or sodium problems. Long-term follow-up with endocrine care keeps dosing on track and checks for related pituitary issues.
This page collects articles and resources related to central diabetes insipidus and nearby topics like medication options, diagnosis guides, and lifestyle tips. Use the links to read deeper on tests, desmopressin dosing, and what to expect after pituitary surgery. If you have questions about treatment, talk to an endocrinologist — they handle hormone problems and will guide you safely.
Monitoring notes: keep a simple daily log of weight, fluid intake, and urine output for a week after any dose change. Sudden weight gain might be water retention; sudden weight loss suggests dehydration. If sodium levels change, symptoms include headache, nausea, confusion, or seizures — report them away. Pregnant people with CDI need extra monitoring; pregnancy can change desmopressin needs.
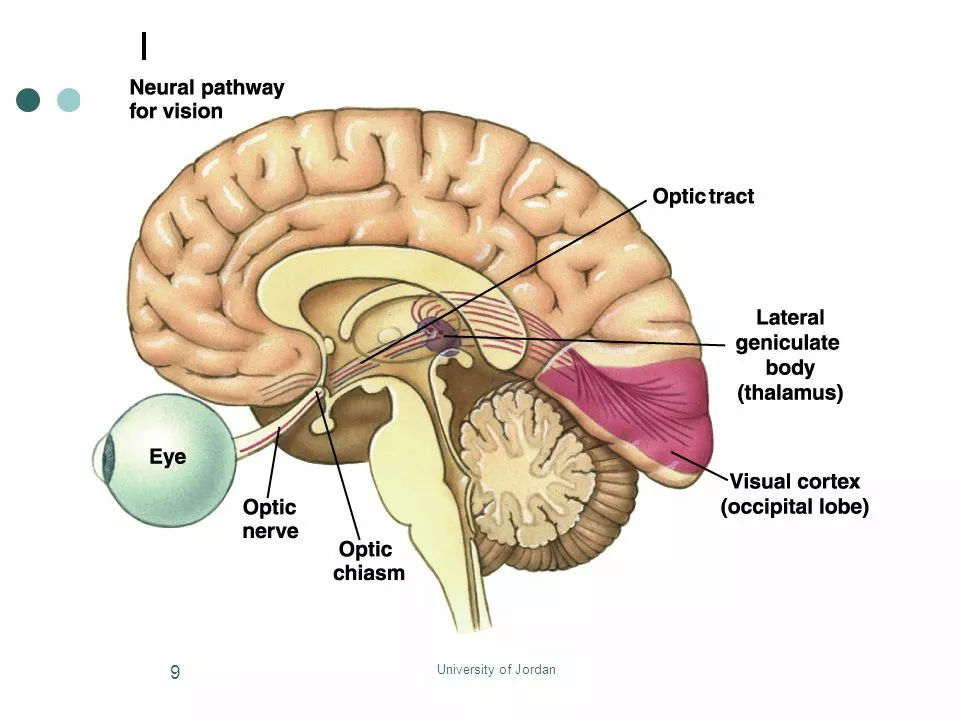
Central Cranial Diabetes Insipidus and Vision Problems: Causes and Solutions
Haig Sandavol May 13 17As a blogger, I've recently researched the connection between Central Cranial Diabetes Insipidus (CCDI) and vision problems. CCDI is a rare medical condition that affects the production of the antidiuretic hormone, which can lead to vision issues. The main causes of these vision problems include optic nerve damage, tumor growth, and inflammation. To address these issues, treatments such as hormone replacement therapy, surgery, and medication adjustments may be necessary. It's crucial for individuals with CCDI to consult with their healthcare provider to determine the best course of action for their specific situation.
More Detail